















Team.

cand. Dr. Ing.
Simon Schreynemackers
Co-Founder / Data Scientist
Machine-Learning &
Signalanalyse
schallakustischer Biosignale

B.Sc.
Atrin Pashaei
Co-Founder / Business Development
Markteintritt, Skalierung & strategische Partnerschaften

cand. Dr. Ing.
Luis Wenner
Doktorand
KI-gestützte Optimierung & Finetuning LLM

Dr. biol. hom.
Carlos A. Fonseca Ulloa
Berater
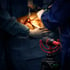
Hüftendoprothesen gehören zu den häufigsten Operationen in Deutschland.
Bei diesem Eingriff wird die Prothese so im Oberschenkelknochen verankert, dass sie stabil sitzt (der „Fit“). Dafür werden spezielle Hammerschläge ausgeführt (der „Hit“). Diese müssen kräftig genug sein, damit die Prothese sicher einrastet, dürfen den Knochen aber nicht beschädigen. Jeder Schlag beeinflusst die Haltbarkeit der Prothese. Je besser der Hit, desto besser der Fit.
Bisher verlassen sich Operateurinnen und Operateure dabei vor allem auf Erfahrung, das haptische Feedback und ihr Gehör.
Hier setzt Fit ωith Hit an:
Unsere KI analysiert in Echtzeit die Implantationsgeräusche von Prothese und Hammer. Sie erkennt kritische Situationen, gibt unmittelbar Warnsignale und dokumentiert die Qualität der Schläge. Damit unterstützt sie das chirurgische Team, erhöht die Patientensicherheit und soll helfen, Komplikationen und vorzeitige Wechseloperationen zu vermeiden.
Wo stehen wir gerade?
Fit with Hit baut auf einem patentierten Verfahren zur akustischen Echtzeitanalyse bei der Hüftendoprothetik auf. Nach ersten klinischen und biomechanischen Ergebnissen entwickeln wir das System derzeit in Richtung multizentrischer Validierung, robuster Echtzeitfähigkeit und regulatorischer Anschlussfähigkeit weiter. Die aktuelle Datenerhebung erfolgt in unseren Pilotzentren am UKGM Gießen und am Pius Hospital Oldenburg. Parallel arbeiten wir an der technischen Plattform, der standardisierten Aufnahmeinfrastruktur und der Vorbereitung des regulatorischen Pfads.
Wie sieht die Timeline aus?
Aktuell:
Datenerhebung in den Pilotzentren und methodische Weiterentwicklung im Forschungstransfer.
2026 bis 2027:
Wissenschaftliche Validierung über mehrere Prothesentypen, Ausbau der technischen Infrastruktur sowie Vorbereitung der Grundlagen für weiterführende Transferschritte.
Ab 2028:
Weiterentwicklung im Rahmen angestrebter Förderprogramme, insbesondere im Forschungstransfer, mit Fokus auf Studienvorbereitung und klinische Translation.
Perspektivisch
Schrittweise Überführung der Forschungsergebnisse in weiterführende Validierungs- und Zulassungsvorhaben.

Operationen müssen nicht nur durchgeführt, sondern auch dokumentiert werden.
Während oder nach dem Eingriff werden Berichte diktiert oder manuell erstellt, anschließend codiert und ins Krankenhausinformationssystem (KIS) übertragen.
Das kostet wertvolle ärztliche Zeit, verzögert die Verfügbarkeit von OP-Berichten und kann zu Dokumentationslücken führen.
Hier setzt OPtimus an:
Unsere KI erfasst während der Operation Sprache und Geräusche, erkennt automatisch die einzelnen Phasen des Eingriffs und erstellt daraus einen strukturierten, OPS-codierfähigen OP-Bericht. Dieser Bericht liegt unmittelbar nach dem Eingriff vor und kann direkt in das KIS übernommen werden.
Wo stehen wir gerade?
OPtimus befindet sich aktuell in der Pilot- und Validierungsphase. Unser System wird bereits in ersten realen Versorgungsszenarien getestet und weiter für den klinischen Alltag geschärft. Im Fokus stehen dabei die zuverlässige Erkennung von OP-Phasen, die automatische Strukturierung des Berichtswesens sowie eine belastbare OPS-Kodierunterstützung für orthopädische Eingriffe.
Wie sieht die Timeline aus?
Parallel arbeiten wir an der technischen und regulatorischen Weiterentwicklung, damit OPtimus 2027 sicher, integrierbar und praxistauglich in bestehende Krankenhausprozesse eingebunden werden kann. Ziel ist eine On-Prem-Health-App mit Anbindung an bestehende HIS-/KIS-Strukturen, die Dokumentationsaufwand reduziert, Transparenz erhöht und klinische Teams im OP spürbar entlastet.
Publikationen.
Acoustic Prediction and Biomechanical Validation of Primary Stability in Uncemented Short‐Stem Hip Prostheses: An Experimental Study
DEz
2025
Alexander Jahnke*,
Simon Schreynemackers*, Ahmed Tawous , Swantje Petersen,
Samar Hamad, Markus Rickert,
Bernd Ishaque
Introduction: In uncemented hip arthroplasty, achieving sufficient primary stability is essential for long‐term implant success. However, objective intraoperative assessment of fixation quality remains challenging. Acoustic analysis of stem impaction sounds offers a promising tool for real‐time evaluation, but its diagnostic accuracy and biomechanical correlation require further validation.
Methods: Twelve formalin‐fixed human femora were implanted with cementless Metha short stems under three predefined anchorage conditions: loose, optimal (fit), and fracture‐inducing press‐fit. Impaction sounds were recorded using calibrated microphones and processed via frequency‐domain analysis. Relative micromotions were quantified under torsional loading to biomechanically assess primary stability. Spectral markers reliably differentiated between anchorage states.
Results: The transition from loose to fit showed minimal spectral change, yet emerged as statistically significant across multiple frequency clusters, while fit‐to‐fracture was characterized by a significant increase in low‐frequency energy (<2.5kHz) and pronounced attenuation in high‐frequency bands (>15kHz). These acoustic signatures closely correlated with biomechanically measured micromotions, which showed a distinct hierarchy: fracture < fit < loose. Cluster permutation analysis confirmed statistically significant differences between all groups, particularly in the fracture condition.
Discussion: This in vitro study demonstrates that frequency‐based acoustic analysis can distinguish between stable, insufficient, and over‐press‐fit conditions during stem implantation. The findings support the feasibility of intraoperative acoustic monitoring as a real‐time, objective tool to enhance implant safety and detect cortical compromise at an early stage, before clinical manifestation. However, translation into a clinical product will require further algorithmic development, integration into a surgical interface, and prospective in vivo validation.

Acoustical determination of primary stability of femoral short stem during uncemented hip implantation
22
Aug
2023
Carlos A. Fonseca Ulloa, Simon Schreynemackers, Torben Harz, Frieder W. Lang, Christian Fölsch, Markus Rickert, Alexander Jahnke, Bernd A. Ishaque
Background: Preparing the medullary space of the femur aims to create an ideal form-fitting of cementless implants to provide sufficient initial stability, which is crucial for osseous integration, ensuring good long-term
results. Hammering the implant into the proximal femur creates a press-fit anchoring of the endoprosthesis in the medullary space. Implanting the optimal size of the shaft for best fitting should avoid damage to the bone.
Modified acoustic signals in connection with implantation are being detected by surgeons and might be related to the primary stability of the implant.
Methods: This study aims to explore the relationship between frequency sound patterns and the change in stem stability. For this purpose, n = 32 Metha® short stems were implanted in a clinical setting by the same surgeon. During implantation, the sounds were recorded. To define a change in the acoustic system response during the
operation, the individual blows of the implantation sequence were correlated with one another.
Findings: An algorithm was able to subdivide through sound analysis two groups of hammer blows (area 1 and area 2) since the characteristics of these groups showed significant differences within the frequency range of 100 Hz to 24 kHz. The edge between both groups, detected by the algorithm, was validated with expert surgeons’ classifications of the same data.
Interpretation: In conclusion, monitoring, the hammer blows sound might allow quantification of the primary
stability of the implant. Sound analysis including patient parameters and a classification algorithm could provide
a precise characterization of implant stability.

Founding.
Wir sind stolz darauf, mit unserem Startup Teil der hessischen KI-Innovationslandschaft zu sein und durch renommierte Programme gefördert zu werden.
Go-Bio Initial
Wir sind stolz darauf, dass unser Startup im Rahmen des Programms GO‑Bio initial gefördert wurde. Das von der Bundesregierung geförderte Programm unterstützt innovative Forschungsprojekte dabei, ihre Ideen in praktikable, marktfähige Lösungen zu überführen und den Weg in die Wirtschaft zu ebnen.
Unser Projekt baut auf einem hochrelevanten medizinischen Anwendungsfeld auf und verfolgt das Ziel, eine praxisnahe Innovation mit messbarem Mehrwert für Patient:innen und Behandlungsteams zu entwickeln. Die GO‑Bio‑initial‑Förderung ist für uns ein wichtiger Schritt auf dem Weg von der Forschungsidee zur marktfähigen Produktlösung.
Hessischer Ideen Stipendium
Wir sind stolz darauf, mit unserem Startup in das Halbfinale des Hessischen Gründerpreises 2022 eingezogen zu sein. Der Preis würdigt junge Unternehmen aus Hessen, die nicht länger als fünf Jahre im Markt sind und durch innovative Geschäftsmodelle überzeugen.
Unser Projekt wurde in der Kategorie Gründung aus der Hochschule ausgewählt, was die hohe Bewertung unserer Idee und ihres Potenzials im akademischen sowie wirtschaftlichen Umfeld reflektiert. Die Teilnahme am Halbfinale war ein wichtiger Meilenstein auf unserem Weg von der Forschungsidee zur marktfähigen Lösung.










